 |
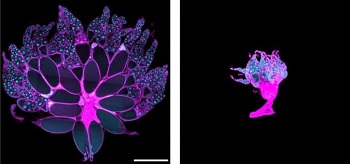
| Mouse ovaries in a healthy mouse and a mouse with tumors--Courtesy of UC Berkeley |
A pair of research teams at UC Berkeley and Harvard has come up with some new avenues of research that hold the promise of finding new drugs to treat cachexia, the deadly wasting disease that afflicts cancer patients.
About one in 5 cancer patients die from wasting as healthy tissues shrivel as tumor cells proliferate, making it a major, if puzzling, focus in oncology.
Two teams, one involving Bilder and Alejandra Figueroa-Clarevega of UC Berkeley and the other led by Norbert Perrimon of Harvard Medical School and his collaborators, centered on the genetics of the fruit fly to try and come up with an explanation. They concluded that there was a tumor-secreted molecule--ImpL2--that caused fat, muscle and ovaries to waste away.
ImpL2 is represented in mammals by insulin growth factor binding proteins (IGFBPs) which interfere with the way glucose is absorbed in muscles and fat. Depleting ImpL2 prevented wasting in fruit flies, and finding the right approach for IGFBPs has promise for humans.
"Because humans have several homologous IGFBPs, the studies suggest new candidates for mediators of cachexia, which could point to novel therapeutic approaches," Bilder says. "If specific IGFBPs could be identified that mediate cachexia from certain tumor types, then blocking those proteins could offer a more targeted and effective approach than systemically administering insulin, which risks stimulating tumor growth."
Harvard Medical School's Young Kwon, the lead author on the second study, also observed that proliferating tumor cells escaped wasting syndrome by consuming a large portion of the available glucose, which helped drive the disease in the rest of the tissues involved in cachexia.
- here's the release
- get the abstracts for the Figueroa-Clarevega and Bilder paper and the Kwon et al. paper