Alzheimer's has long been one of the most contentious fields in drug development. As one drug after the next failed in late-stage clinical studies, drug developers have been moving further and further upstream in the disease process to see if they can more effectively blunt the progress of this disease in early-stage patients. And that shift has focused a bright spotlight on finding better ways to diagnose Alzheimer's early on as the currently used crude methods leave much to be desired.
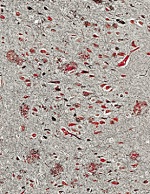 |
| Micrograph of amyloid plaques and neurofibrillary tangles in human brain.--Courtesy UCSD |
A new study from UC San Diego School of Medicine, though, suggests that finding the right biomarkers will be challenging as early indicators for Alzheimer's aren't fixed for all patients.
"Our current ability to identify early stages of AD is limited by the focus on amyloid accumulation and the expectation that biomarkers follow the same timeline for all individuals," said Emily C. Edmonds, a senior postdoctoral fellow in the Department of Psychiatry. But she added that "AD is complex in the sense that there may be different neurobiological pathways leading to expression of the disease. Our findings suggest that the number of abnormal biomarkers and cognitive markers an individual possesses, without regard to the temporal sequence, is most predictive of future decline."
Studying 570 cognitively normal people in the Alzheimer's Disease Neuroimaging Initiative, the investigators determined that evidence of neurodegeneration was much more common that amyloid accumulation at baseline. Shifting the focus to a group of patients with mild cognitive impairment, evidence of neurodegeneration, amyloid accumulation and "subtle cognitive decline" all played a role in flagging the disease early on.
"At present, it is much more common for assessment of cognition to be based on insensitive screening measures or reports of cognitive problems by patients or their family members," said Edmonds. "These blunt screening tools can be very unreliable, which might explain why cognitive decline has traditionally been viewed as occurring later in the disease process. The integration of sensitive neuropsychological measures with assessment of biomarkers of AD can enhance our ability to more accurately identify individuals who are at risk for future progression to AD."
- here's the release