 |
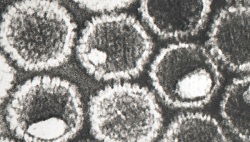
| Herpes simplex virus--Courtesy of CDC |
By turning their backs on years of research work on fighting herpes viruses, Howard Hughes Medical Institute investigators at Albert Einstein College of Medicine say they were able to design a radically different type of vaccine that proved effective in mice. And they say the same vector has promise in fighting diseases like HIV and tuberculosis.
In the past, says the team, researchers have focused on developing vaccines that targeted the glycoprotein gD, which is found in the viruses outer layers. The glycoprotein is required for the spread of the microbe, while also responsible for kickstarting the production of antibodies.
The team, though, decided to develop a mutant which deleted gD, and found that a deleted HSV-2 virus could get into a cell, but couldn't spread. And those cells became very effective at producing antibodies that completely immunized lab mice against HSV-2--currently a lifelong infection for hundreds of millions of people--with the antibodies attaching themselves to the cells and signaling for a white blood cell attack that destroyed the target.
"It was necessary to shake the field up and go another route," says Betsy Herold, a virologist and infectious disease physician at the Albert Einstein College of Medicine and co-study leader of the new research. "It's possible we could clone into this HSV vector pieces of other viruses, such as HIV, and maybe the immune system would produce the same types of ADCC antibodies for those viruses."
"With herpes sores you continually get them," says HHMI investigator William Jacobs. "If our vaccine works in humans as it does in mice, administering it early in life could completely eliminate herpes latency." Jacobs and his colleagues reported their findings on March 10, 2015, in the journal eLife.
- here's the release